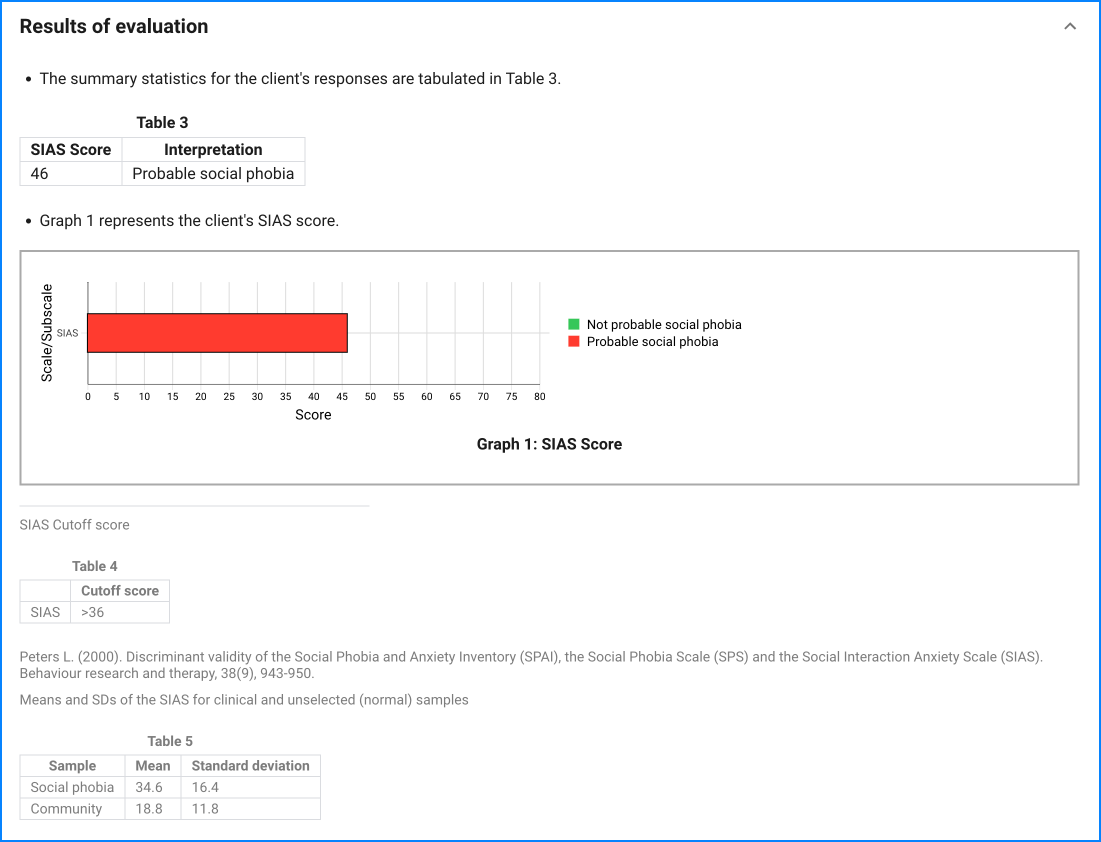
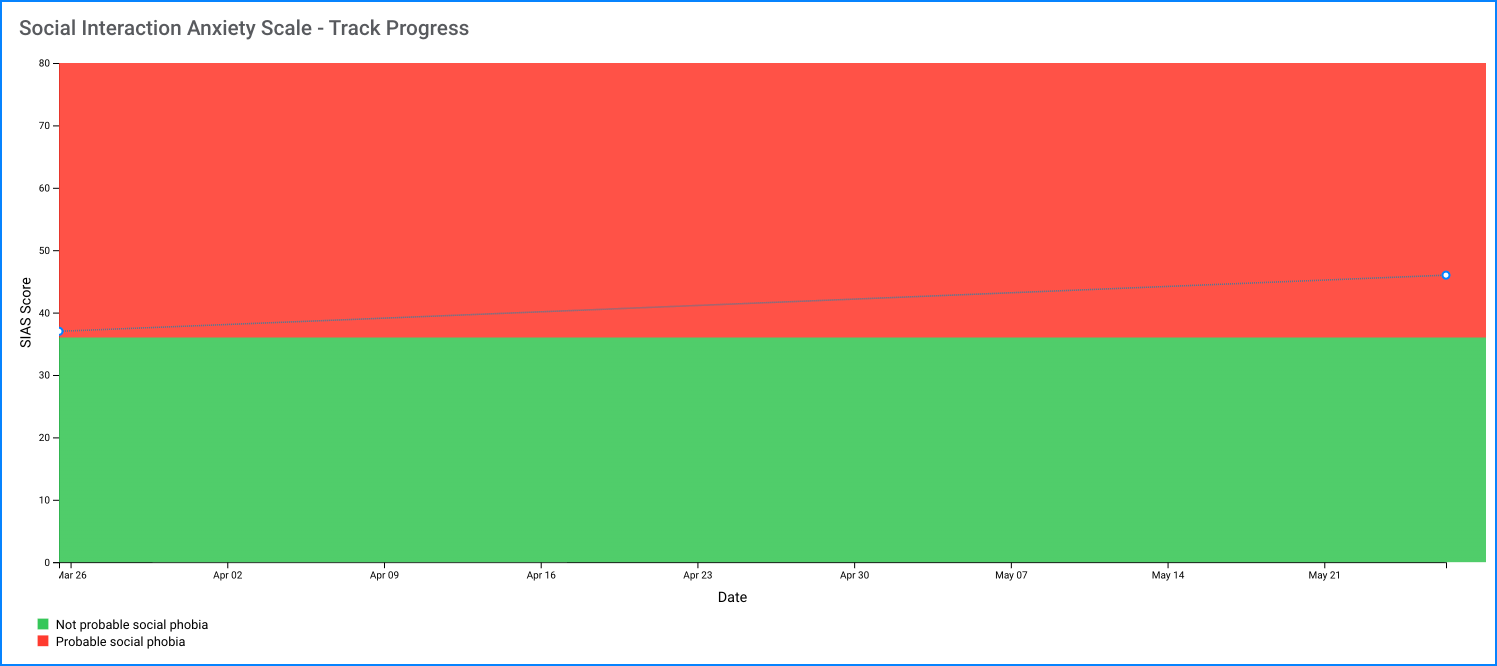
Since the questionnaire relies on client self-report, all responses should be verified by the clinician, and a definitive diagnosis is made on clinical grounds taking into account how well the client understood the questionnaire, as well as other relevant information from the client.
The Social Phobia Scale (SPS) and the Social Interaction Anxiety Scale (SIAS) were developed as a companion set of measures by Mattick and Clarke in 1998. The scales correlated well with established measures of social anxiety, but were found to have low or non-significant (partial) correlations with established measures of depression, state and trait anxiety, locus of control, and social desirability. The scales were found to change with treatment and to remain stable in the face of no-treatment.
However, there are at least three limitations to the scales. First, while social desirability factors do not seem to affect the responses given to the scales, subjects can, if they wish, fake their responses. Secondly, most of the items are scaled in the same direction, increasing the possibility of a response bias. With regard to this second point, it is noted that the scales still seem sensitive to differences between clinical groups, suggesting response bias problems may be minimal. Thirdly, the correlations between the SPS and established measures of social anxiety were quite high, raising the issue of why a measure of social phobia scrutiny fears correlates well with a measure of social interaction anxiety. It would seem that social phobia scrutiny fear frequently (although not necessarily always) coexists with social apprehensiveness more generally. This finding is not surprising and is consistent with clinical observation (e.g. Biran, et al., 1981; Nichols, 1974) and empirical research (e.g. Turner et al., 1986).
The SPS and SIAS are proposed to be used as companion measures to allow a comprehensive assessment of social phobia fears. The new scales assess different aspects of the disorder and, despite the fact that they show a high intercorrelation, they should not be viewed as interchangeable. Subjects who have a low score on the SPS may score highly on the SIAS, and thus a therapy for a focal phobia (e.g. writing fear) would be at risk of failing to assess the background concerns tapped by the SIAS, and vice versa. The authors recommend that the scales be used together. It may be that the separate analysis of these related constructs will yield a more sensitive evaluation of any (differential) treatment effects achieved by active therapy for this disorder.